Kaj and Poppy’s Birth Story
I write this the eve before their first birthday (posted 2 months later), how did that happen so fast? Here goes, and sorry, but I’m pretty blunt and won’t be sugarcoating much of the gory details–you’ve been warned. It was a dark and stormy night. Just kidding, it wasn’t really, although the weather had been lovely and chilly and we had firewood on the ready. I always thought I would embrace every aspect of pregnancy and wouldn’t be one who complained. That was until I began having severe heartburn at just ten weeks that only increased and worsened throughout my pregnancy. That was my only real big complaint. Because of this, I had been sleeping upright on the couch for about 6 weeks or so. I could no longer sleep in bed. I was FORTY WEEKS AND FIVE DAYS on Friday, December 2nd, so over it and getting desperate. My husband was going to possibly be starting a 6-week job that he could not miss and the thought of him missing their birth had me in tears.
Friday, December 2nd, 10:56 am
Me to Dr. Stu via text: “So, I’m in tears. Richie has a potential six-week driving job that would start Monday, he should know for sure at the end of today. What if he misses the birth? (sad face emoji) if nothing is happening today should we do another sweep? Any other suggestions to get them moving?”
Dr. Stu’s reply: “I have no definitive answer for you. Yes. I can do another sweep. You always have the option of hospital induction. I know that sucks but it has to be considered in the mix.”
Me: “Okay, thanks. Induction is out of the question. Will keep working on things and trust.”
So I decided to try an “induction smoothie” that a little birdie had told me about. It consisted of almond butter, apricot nectar, castor oil (not a lot) and lemon verbena. I tried it thinking honestly that it wouldn’t work. I found out weeks later that my doctor was not too thrilled with my choice, or maybe more so not too thrilled with my choice not to tell him. Oops, sorry! But I really honestly didn’t think it would work. It was more of a last-ditch effort to say I did what I could do. I drank the smoothie around 5 pm that day, Friday the 2nd. We had a nice hearty meal that night. My mom who had been staying with us for 3 weeks already in anticipation that I would deliver early because I was carrying twins, made a delicious shepherd’s pie. I even posted on social media about that meal hopefully being my “last supper” before I went into labor.
7:25pm
Me to Stu: “This probably means nothing but in the last couple of hours or so my cervical fluid has been clear like egg whites, twice when I’ve wiped, a decent amount. Having minor period type cramps.”
Stu: “Good. Hopeful. Any blood?”
Me: “Not fresh”
Stu: “Maybe leaking water. We will see.”
Me: “Wouldn’t it be making my undies wet if I was leaking water?”
Stu: “Depends on if leaking or actually ruptured. But with a low head sometimes it can trickle. Just rest. Drink. Eat. And be merry.”
Me: “Been having lots of water, about to have a glass of wine and shepherd’s pie with the fam.”
Stu: “Ok.”
We all finally went to bed around 11 pm and I figured, well, that smoothie was stupid, it didn’t do anything. I fell asleep in my little nest on the couch, upright of course, only to wake a couple of hours later.
Saturday, December 3rd, 2:33 am
Me to Stu: “I’m having contractions about 4 minutes apart, lasting 45 seconds to a minute. They’re somewhat intense but for now, I’m managing them on my own (Richie and my mom are sleeping). It sort of comes up from below and wraps around my belly and low back.”
Stu: “Any bloody show or more leakage?”
Me: “No blood, hard to tell about leakage, I have to pee pretty often.”
Stu: “Ok. Babies moving some?
Me: “A little.”
Stu: “Ok. This is great. How long have they been every 4?”
Me: “I think for about 45 minutes. Now they’re a little more like 3 minutes, but they’re still manageable.”
Stu: “Ok. If they stay that way for another hour or two or if you see bloody show sooner then let me know. Try to rest in between. Keep hydrated.”
Me: “I’m using a tracker but it doesn’t say when I started. Ok.”
Stu: “See you soon. Yay!”
Me: “They seem to be getting closer together will keep you posted.”
Stu: “That’s what should happen.”
Me: “But again, still manageable on my own for now.”
3:19 am
Me: “They’re definitely getting intensely stronger and closer, about 2.5 minutes apart.”
Stu: “Ok. I’ll mobilize everyone. See you in a bit.”
Me: “I’m nervous it will be a false alarm and you come all this way.”
Stu: “Not to worry. Clear your mind. Still no blood?”
Me: “Yep, just wiped fresh blood!”
Stu: “Okay, see you in a bit. ETA 4:10.”
At this point, I could no longer quietly labor on my own and Richie and my mom had woken up to my moans. I had also contacted my friend Hillary who has had 4 babies of her own but had never witnessed a birth and asked if she could be there. I adore her, so of course, I didn’t mind. She came over right away. Next on the call list was my friend Claire who would be my photographer for the big event and my dear friend Katie who is studying to be a midwife and asked if she could attend. I was more than happy to have these women by my side as extra support.
Stu and his team, Beth, Blyss, and Catalina arrived right around 4 am. They got the birth tub started right away. I labored in my bathroom in the meantime, the only renovated room in the house, hence my favorite room in the house. Things seemed so intense so fast that I thought for sure I would be pushing these little ones out in no time. But alas, that was not their plan. Before I knew it the sun was coming up and I was still laboring away in the birth tub that was set up in the dining room. Thank God for warm water and a birth tub by the way, what a difference it makes!

I want to get back in the fucking tub!
By around noon my contractions had slowed quite a bit to about 7 minutes apart and Dr. Stu wanted me to get out of the tub for a while to see if we could get things moving again. I was not thrilled about this idea but of course, I obliged. I moved back to my favorite room and labored on the toilet for a while, that was not fun and being out of the water really increased the intensity of the contractions, like REALLY increased the intensity. I don’t know how laboring out of the water is doable the whole time, yikes! I then moved to the shower and sat on the birth ball as the hot water hit my back. Still not the same as that birth tub but better than no water. I’m not sure how long it was that I was out of that tub but it seemed like an eternity. It felt like hours but was likely less than a half an hour, I don’t really know. I vaguely remember repeatedly asking Hillary to rub more Valor essential oil on me, it helps with bravery and confidence, I was in need of both. As my contractions started up again I remember saying with pure intent, “Sorry guys, I’m getting back in the fucking tub.”
I’m not sure at what point he checked me, I can’t remember if it was before or after I got out of the tub but I remember being a little disappointed that I wasn’t farther along. I continued to labor in that glorious hot water in my dining room with my mom and my dear friends and my dream birth team by my side. Being given coconut water, regular water, juice, popsicles and chia seed bars every now and again. Our dog Hugo would come in and check in on me now and again and give me a little lick. My husband being the kind man that he is would offer a cup of tea here and there to everyone and was there to support me while giving me space all at the same time. I had moments of wanting to break down and give up and cry my eyes out like I used to do so often as a little girl. I can remember saying here and there to Katie, “Are you sure I can do this? I don’t think I can fucking do this.” And she would gently remind me that I am doing it.

Keeping Richie hydrated.
The time came that Stu wanted to break my water to attempt to move things along. I was reluctant and fearful but Beth and Blyss talked me through my fears and I decided to do it. It wasn’t too terribly long after he broke Baby A’s bag of water that I was complete and Stu said I could start to push. Towels were placed by the fire to start warming and Richie got in the tub with me. He got behind me and really helped give me some leverage but pushing was not easy.

Are you fucking kidding me right now?
I pushed so hard that yes, the inevitable happened, I pooed a little bit in the tub. Sounds horrifying but it really wasn’t. They quickly scooped it out with the little fish net scooper and that was that. I tried pushing for a bit, maybe an hour, maybe less, maybe more? What I do know is that it was so hard and if I’m being honest with myself I feel like I was holding back just the tiniest bit for fear of tearing so bad that I would never recover. As it turns out my boy’s head was tilted in such a way that he was having a difficult time making his way. He was asynclitic. Stu suggested that the tub was not the ideal space to deliver and that we should move to the bedroom and consider using the vacuum. I am usually not one to be pro vacuum but it was like music to my ears. I remember responding immediately, “Yep, let’s do it”. So we headed to the bedroom in between contractions. I’m not going to lie, the delivery was intense. It all suddenly seemed to speed up and become less of a drama-free float in the water to “holy shit, what is happening right now?”.

Baby Boy is finally here!
He secured the vacuum on my son’s head and pulled while I pushed only for the vacuum to pop off three times! I feel like I was in another world and on the fourth time I remember thinking in my head, “Maybe you should push harder this time.” It was like something inside of me said, “This is it, now or never, push him out now!” It was the worst and best feeling all at once. Oh the pain but oh the relief. And then suddenly, he was here, my Kaj Joaquin, born 8 pounds 4 ounces at 3:51 pm on December 3rd. He was gorgeous! A full head of dark brown hair, the source of my heartburn according to the old wives tales. I was immediately in love.
The next few minutes were otherworldly, like I think I pretty much left my body for moments at a time. I saw that Dr. Stu was looking concerned and I remember asking as they were monitoring “Baby B’s” heart rate, “Is she okay?” He responded, “No, she’s not okay. We need to get her out immediately.” Now, this was something he had warned me about in our prenatals, that there was a chance that once Baby A was delivered that Baby B’s heart rate could drop and she would need to come out immediately after. He explained how that would be, but it just sort of went in one ear and out the other because in my heart I just always knew it would all be fine. So here we are, things went exactly as he said they might. Even though she was head down as they prefer second baby to be, she was only negative three station at that point and Big Boy’s cord was now in the way along with her arm so the vacuum was out of the question. Even though he explained what he was about to do, it just all happened so fast and was so intense that I left; bye-bye. I didn’t pass out but I remember leaving my body while at the same time knowing and feeling exactly what was happening. It was the strangest thing and very hard to explain. He had to break her bag of waters, push my sweet girl back up into my uterus, find her feet and flip her around and pull her out by her feet. So even though she behaved and stayed head down as she was supposed to, I guess I can still say I vaginally delivered a breech baby. But really that was all Dr. Stu on that one, he pretty much delivered her, not me. Delivering breech babies is a common occurrence for him but the procedure he did here was not so common and turns out his first time in all of his years of practice. Can I just say how grateful I am that he learned this with his teacher? How grateful I am that he knew exactly what needed to be done and he did it and safely brought my daughter earthside? After the most agonizing pain I have ever endured, there she was, my sweet teeny tiny Poppy Lou. Born 8 minutes after her brother, weighing in at only 4 pounds, 7 ounces. She was so tiny and so not in her body yet. For her, she wasn’t quite ready and she needed some adjusting to her new atmosphere. Beth worked on her for quite a while, breathing into her and handling her with the most gentle energy. It was intense, not going to lie, especially for my mother and friends who were bearing witness to all of this. But I knew she was fine, I just knew. I never had a moment of panic that she wouldn’t be okay. At one point I remember saying to her, “Come on Poppy Lou, you’re tiny but you’re mighty.” Beth encouraged me to keep talking to her. Finally, after a good long while, she was showing signs of being in her body. Now let me be clear, she wasn’t blue, she wasn’t not getting oxygen, she was still attached to the cord and she wasn’t in danger to the point they felt the need to call an ambulance. If they thought she needed medical assistance, an ambulance would have been called immediately. She just wasn’t quite ready to join us, she was adjusting to the transition. She finally came to and was in her body and before I knew it she was on my chest. She was just the sweetest, most petite little thing I had ever seen and again, I was in love. I had infinite amounts of love for these two little beings that were just gifted to me. How can you be ready to do anything, even die for someone you just met?

And just like that, we’re a family of four.
Then came the placenta removal and the cleaning out of my uterus. Ugh! Just when I thought we were done! Let’s just say I was not a happy camper for another few minutes. I remember taking as much as I thought I could take and then as politely as I could, I said, “Stu, you’ve got to get your arm out of my fucking vagina!”. No joke people, no joke. But guess what, it was the best experience of my life and I would do it all over in a heartbeat. All of it, the good, the bad and the ugly. In fact, three weeks postpartum I remember saying excitedly, “I want to do it again!”
I lost quite a bit of blood and was put on an IV drip and had a catheter placed because Dr. Stu didn’t want me getting up at all. I needed to rest and recover. I was put on two weeks bedrest. It took me a few days to be able to even safely walk to the bathroom alone. I didn’t shower for over a week because of concern of the hot water affecting my blood pressure, which I was totally fine with oddly enough. That first shower was heavenly though!

Mom and Kaji Boy.
I am so grateful for the support I had immediately after their delivery because lord knows we needed it. My sister came to stay and gave skin to skin to Poppy all night on the first night. My mom, thank God for my mom! She whipped up charts and counted pee and poo diapers, and made sure the babies got their donor milk every hour as needed. I quite honestly owe it to my mom for keeping them alive. My friend Daisy who was the saint that had given me some of her milk a few weeks prior in preparation, knowing that Poppy was weighing small. She also brought over a breast pump and a scale to keep track of Poppy’s weight gain the day they were born. Stu brought a giant bag of donor milk the following day from a former client of his. My friend Julie helped arrange donor milk pickups. The community really came through to keep me babies fed and I am forever grateful. Because I lost so much blood it took a very long time for my milk to establish. It was an uphill battle that I never expected. I had put so much emphasis on my perfect home birth that I didn’t prepare for making successful breastfeeding happen. I will do another post on my breastfeeding journey because it deserves its own post. I am happy to say that we made it through and we are still going strong. My friend Abigail Morgan gave me acupuncture treatments. My chiropractor and friend Kolleen came and gave the babies and me adjustments. Friends brought meals. I feel blessed. My postnatal care with my team was topnotch, they came to check on me several times throughout the next couple of weeks.
After experiencing all of this, I feel I can do anything. I am stronger than I ever imagined. My babies, Dr. Stu, and my entire birth team gave me that gift. I hope you have enjoyed this little birth story. I am sure it will be met with both support and judgment and that is okay. I am so truly grateful that Dr. Fischbein allowed me a choice in how I delivered my babies and I wouldn’t change a single aspect of it. I am an open book and happy to address any questions. Here is also a great piece that Dr. Fischbein wrote after their delivery, along with two of his other clients. It is a great read from his perspective. As well, here is an episode of his podcast that I recently had the pleasure of being a guest on. Happy birthing Y’all! #twinning

Together again in their new atmosphere.
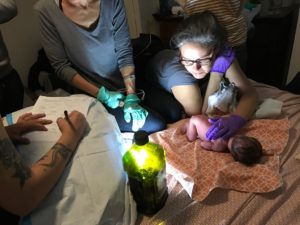
The midwives doing their thing. These women are saints.

Poppy getting measured.

Little Poppy and Dr. Stu. This is one girl he will never forget.

Richie and Dr. Stu weighing the babes at a postpartum home visit.

